Mumbai, 23rd March 2022
In 2008, archeologists had uncovered two 9000-year-old skeletons which were found to be infected with Mycobacterium Tuberculosis that causes Tuberculosis or TB. How has this pathogen persisted for so long?
Today, TB is still one of the most infectious killers, causing more deaths than malaria or AIDS. Further, India accounts for around 26% of the total TB cases across the world. As we observe World Tuberculosis Day on 24th March 2022, here are some important facts about the disease and its treatment.
Expert speakers Dr. Somashekar. N, Director, National Tuberculosis Institute (NTI), Bengaluru and Dr. Ravichandra C., Chief Medical Officer (SAG), NTI Bengaluru shared the below information during a webinar (https://youtu.be/X4OivuFPj60) conducted by PIB.
Q) Is Tuberculosis Curable?
If the patient takes the right drugs for the right duration without any interruption, yes. TB is completely curable. But if there is no proper adherence to drugs, then the patient can even die of the disease. – Dr. Somashekar. N., Director, NTI
Q) Why the Treatment for TB takes so long?
For complete cure, the patient should strictly take TB drugs for a minimum of six months; based on the type of TB, this treatment period may be longer as well. This is because the bacterium Mycobacterium Tuberculosis progresses slowly, divides very slowly and it takes a long time for it to progress from a mere infection to TB disease. This is why long therapy is needed.
Even if the culture results obtained after two months of taking the drugs are negative, the metabolically inactive latent bacilli can harm the patient when they become active. If the drug-levels are not maintained regularly, whenever the latent bacteria become active, there are bigger chances of relapse. Hence the drugs need to be consumed for a longer period, so as to avoid any such instance.
“Even if I am infected with TB today, it takes minimum six months for me to catch the disease. This can sometimes extend even up to 60 years.” – Dr. Somashekar. N, Director, NTI
Q) TB Treatment
TB drugs are not given directly to patients; they are provided under supervision, called Directly Observed Treatment, Short-course (DOTS) therapy. This is because, like every chronic disease, TB drugs are to be taken only till the symptoms subside. Medicines should not be continued after that. The treatment thus needs a patient-centric approach. Under this system, ‘Treatment supporters’ will keep the drugs and the patient has to visit every day and take the drugs from them.
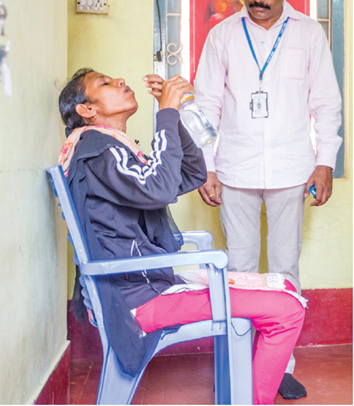
Government Support for TB Patients
Each and every TB drug and diagnosis of TB is free of cost, especially in public sector. Patient need not spend anything. People should come forward and avail the facilities being provided by the government, free of cost. Even if the patient gets diagnosed in a private hospital, the treatment and benefits are the same – Dr. Somashekar. N, Director, NTI

Government of India is providing Rs. 500 per month to all registered and notified TB patients through Direct Benefit Transfer. This support is provided for the treatment duration even if the treatment extends to two years.
The financial support is basically provided to ensure nutritious diet for the patients. High protein diet helps to bring down the adverse effects caused during the treatment and Govt. provides this support to take care of the patients and help them complete the treatment without fail.
Government also provides incentives to Treatment Supporters, who usually are in charge of providing and monitoring the drug intake by patients.
The patient so prefers, he or she can take the treatment in private hospitals as well, but under proper supervision so that they complete the course of the treatment.
In private sector as well, Govt. provides incentives in the form of honorarium to private doctors and nursing homes.
Q) Can Tuberculosis relapse?
Around 10 to 12% of recovered patients can catch TB again; this is called Relapse TB/Recurring TB and is most seen in smokers, alcoholics, and people with uncontrolled diabetes. Undernourishment is another reason.
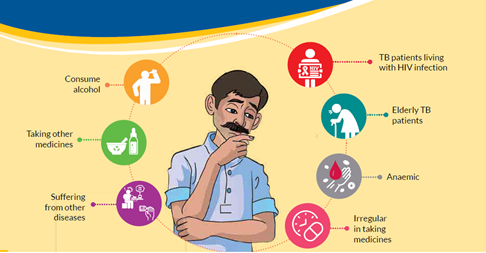
This is why even after completion of treatment, post-treatment follow-up is given where patients visit every six-month up to a period of two years, even if there is no symptom.
If any TB symptom is seen during this period, the patient should immediately approach the doctor.
Relapse TB is also curable –Dr. Somashekar. N, Director, NTI
Q) Is there any correlation between Tuberculosis and COVID-19?
So far there is no evidence of direct relation between COVID-19 and TB. Only area of curiosity is increasing number of Extra Pulmonary TB cases. Wherever there are more COVID-19 cases, more extra pulmonary TB cases are being reported
– Dr. Ravichandra C, Chief Medical Officer, NTI
COVID-19 had a major impact on National TB Programme, since the patients stopped visiting or couldn’t visit hospitals due to the pandemic and resultant lockdowns. There were serious impacts since the resources and personnel allotted for TB were diverted for COVID-19 work.
Even the symptom was same for both the disease – cough. Hence in the initial stage of COVID-19, Government of India issued a circular where the patients who report any symptom of COVID should also be tested for Tuberculosis and vice versa.
Despite that, diagnosis of TB came down drastically. Even when people had cough, they stopped visiting hospitals due to fear of getting COVID or getting isolated. This in turn paved way for spreading of infection to other family members too. Many patients suffered during the Pandemic, which even caused several deaths among TB patients, said the doctors of NTI.
Q) Are there any side-effects of TB drugs?
Any drug if taken for a longer time can cause nausea – Dr. Somashekar. N, Director, NTI
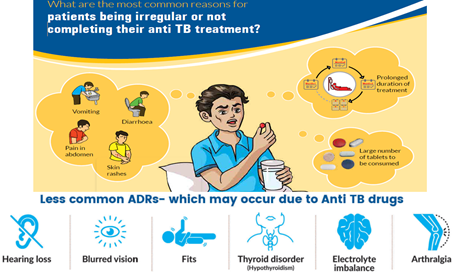
Common side-effects and remedies:
Itching – Use of moisturizer or coconut oil can help
Gastritis – Avoid taking TB drugs on an empty stomach; always take them after food
Blurring of vision – where green leaf appears red to the patient; any change in colour should be immediately reported to the medical officer, who will direct to an ophthalmologist.
Some TB drugs cause Hearing loss and thyroid disorder which may cause joint pain.
All side-effects will settle in two months until our body gets adjusted to it. Continue taking medication until advised by doctor – Dr. Somashekar. N
Note: This is the second part of our press releases on the webinar. Please read the first part here.
***
PIB MUMBAI | DJM/Dhanalakshmi/CY
Follow us on social media: ![]() @PIBMumbai
@PIBMumbai  /PIBMumbai
/PIBMumbai ![]() /pibmumbai
/pibmumbai  pibmumbai@gmail.com
pibmumbai@gmail.com

